Many people may experience discomfort and self-consciousness due to varicose veins. If you are considering getting varicose vein treatment, you should consider how much does varicose vein treatment cost. You might wonder what fees you could pay out-of-pocket and if your health insurance would cover them.
Does Varicose Vein Treatment Fall Under Health Insurance?
Depending on the type of insurance plan you have and the precise therapy your healthcare professional recommends, the cost of treating varicose veins may or may not be covered by health insurance. Generally, if varicose vein therapy is judged medically essential, health insurance may pay for it. The degree of your symptoms and their possible influence on your general health are often used to assess whether a treatment is medically necessary.
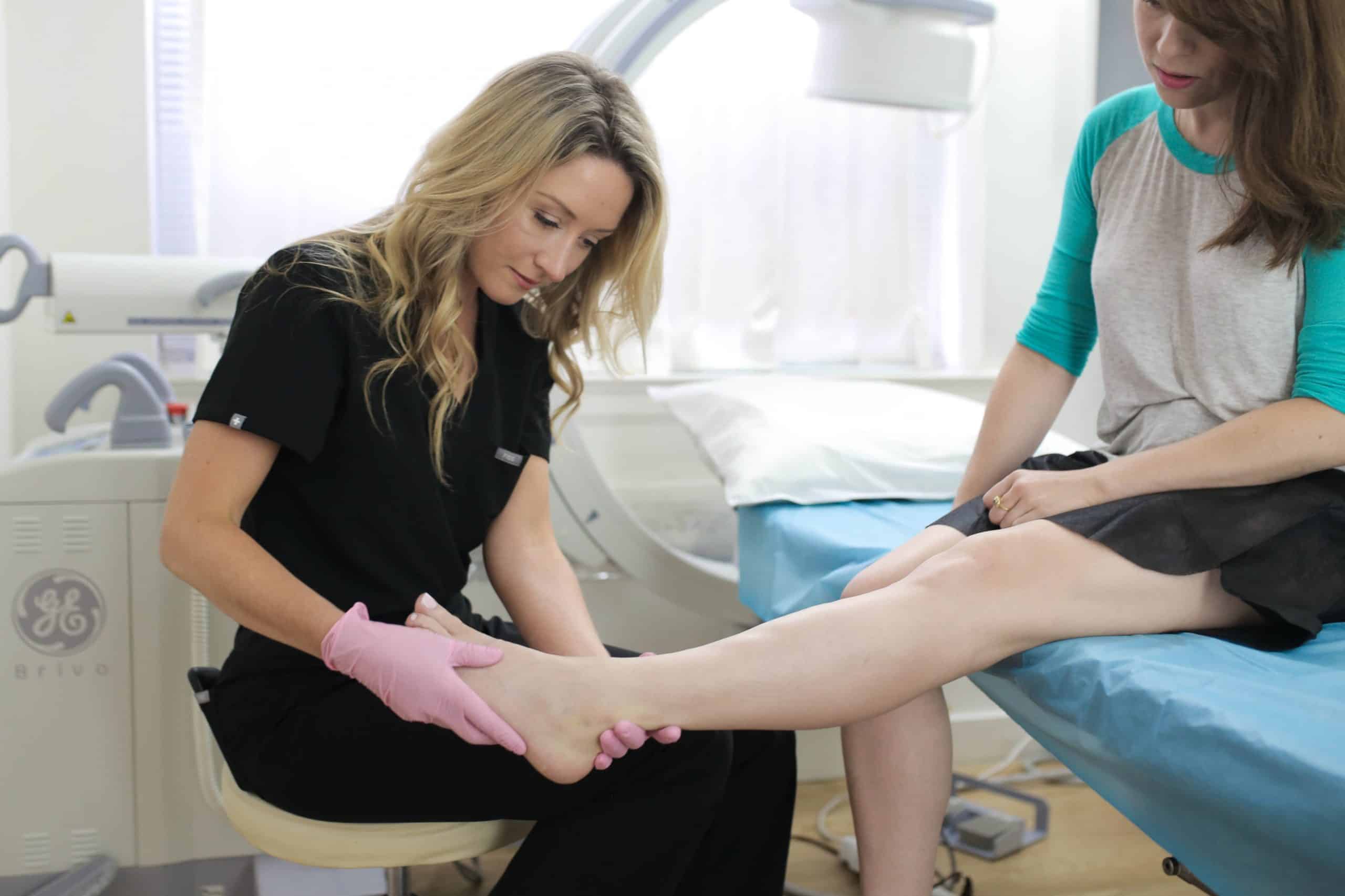
What Kinds of Varicose Vein Treatment Are Insurance Plans Covering?
If they are judged medically essential, the following varicose vein treatments are often covered by health insurance plans:
Evla (Endovenous Laser Ablation)
Laser light is used during the minimally invasive EVLA technique to treat varicose veins. When deemed medically essential, it is frequently reimbursed by health insurance programs as a therapy for symptomatic varicose veins.
Sclerotherapy
Varicose veins are injected with a solution during the non-surgical process known as sclerotherapy, which eventually causes them to collapse and disappear. If the veins are causing substantial problems, this therapy is often covered if medically necessary.
Phlebectomy Ambulatory
A surgical treatment called an ambulatory phlebectomy uses tiny incisions to remove varicose veins. If this treatment is important to reduce symptoms and enhance general health, health insurance could pay for it.
Stockings With Compression
Varicose veins are frequently treated conservatively by wearing compression stockings. They squeeze on the legs to increase blood flow and lessen discomfort. Compression stockings may occasionally be covered by health insurance policies if recommended by a medical professional.
What Are the Patients' Out-of-Pocket Costs?
Although part or all of the cost of treating varicose veins may be covered by health insurance, individuals may still be responsible for out-of-pocket costs. These costs may consist of:
Deductibles
The amount you must pay out-of-pocket before your insurance coverage begins is called a deductible, a feature of most health insurance policies. You will be responsible for paying the entire cost of the therapy up until your deductible is satisfied if you have not reached it.
Co-Insurance Or Co-Payments
Patients frequently have to make co-payments or co-insurance for medical treatments under health insurance policies. Co-insurance is a portion of the overall cost you are responsible for. In contrast, a co-payment is a set amount for each visit or service. These sums may differ based on your insurance plan.
Uncovered Treatments
Health insurance may not cover therapy if it is deemed cosmetic or not medically required. In these circumstances, patients would be responsible for paying for the whole therapy out of pocket.
Summing Up
Patients may still have to pay out-of-pocket costs like deductibles, co-payments, or co-insurance. Before starting varicose vein therapy, reviewing your insurance policy and discussing coverage with your doctor is crucial. Knowing are varicose veins covered by insurance will help you budget for any unforeseen costs and ensure you get the care you need for better vascular health.





